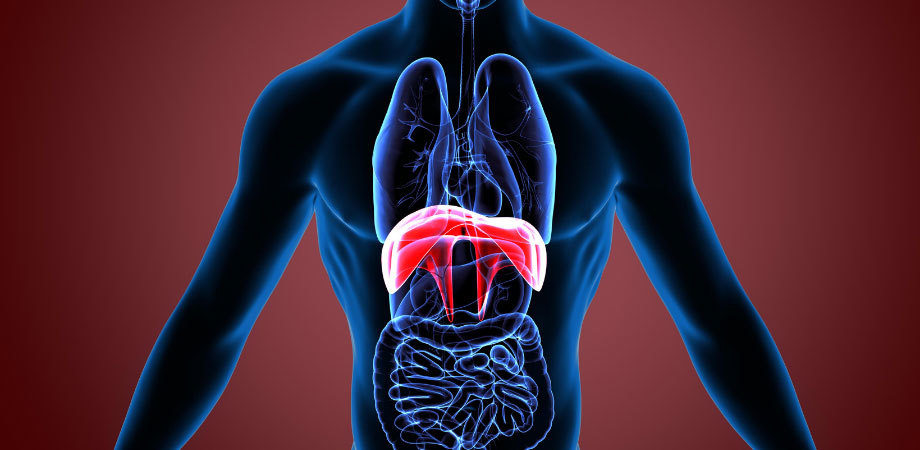
Introduction to Nasal and Diaphragm Breathing
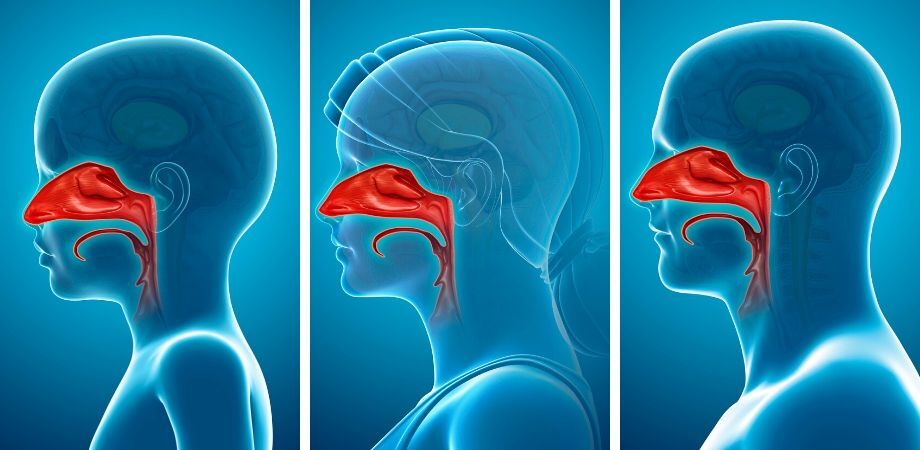
NASAL BREATHING
Why we need to learn how to breathe
James Nestor in Breath: The New Science of a Lost Art, estimates 80% of the world’s population is not breathing correctly. Healthy breathing is breathing in and out through the nose and breathing appropriately for the activity. For example, while it might be appropriate to breathe more when running, it isn’t when you are sleeping. Loud snorers are breathing 2-3 times more air than normal. They are effectively running a marathon in their sleep. By contrast, wild animals are healthy breathers and nose breathers. Horses can gallop as fast as 80 kmph breathing through the nose. Cheetahs have been clocked at speeds of up to 110 kmph, breathing through the nose. Wild animals don’t snore and very rarely get blocked noses. Humans, on the other hand, have the distinction of being the most plugged-up species on the planet.
How to tell if you are breathing incorrectly
Symptoms like nasal congestion, habitual mouth breathing, asthma, hay fever, persistent cough, snoring or sleep apnoea, anxiety or susceptibility to panic attacks may be indicative of a dysfunctional breathing pattern. Anyone who finds nasal breathing uncomfortable probably needs to look at their breathing.
How dysfunctional breathing exacerbates asthma
People with asthma tend to have hypersensitive airways. This means they are more likely to react to sudden changes in air temperature or airborne allergens like pollen, dust, dust mites, strong perfumes, or smoke.
People with asthma tend to habitually over-breathe (hyperventilate) and breathe through the mouth. This is a problem because the nose is a natural air conditioner. It filters, warms, humidifies, and disinfects the air before it is inhaled into the lungs. If we breathe though the mouth, we potentially take cold, dry, unfiltered air directly into the lungs and this can trigger asthma in susceptible people. Chest tightness, inflammation and, in some cases, mucus congestion are often caused and exacerbated by over-breathing and mouth breathing. Nasal breathing also helps optimise levels of the gases carbon dioxide (CO2) and nitric oxide (NO) in airways and blood. Both CO2 and NO are bronchodilators helping to open airways for easier breathing. CO2 and NO also act in a similar way as vasodilators, improving the flow of oxygenated blood in arteries and arterioles. And if that weren’t enough, nasal breathing helps to maintain adequate levels of NO which acts as a germicide and one of the body’s first lines of defence against airborne germs.
One tip to help people better control their asthma
Breathe through your nose. Nasal breathing is more efficient and delivers more oxygen to the body by optimising levels of oxygen, carbon dioxide and nitric oxide in airways and blood. Nasal breathing also helps reduce breathing volume, thereby reducing exposure to airborne allergens.
Why many people with asthma, for example, sometimes find it hard to breathe through the nose.
It helps to think of nasal congestion as asthma of the nose. After all, nasal congestion results from a combination of inflammation and constriction of the nasal mucosa, often accompanied by excessive mucus production, similar to asthma. It may seem odd, but these symptoms can be caused and exacerbated by mouth breathing and over-breathing. One of the best things we can do is try to breathe less air and that starts with practising to breathe gently through the nose.
What to do if your nose is blocked
Here is a technique that may help temporarily unblock your nose. Prior to doing this exercise, check your left and right nostril to see how clear they are.
- Take a gentle breath in through your nose.
- And a gentle breath out through your nose.
- Now hold your breath, closing your nostrils gently between thumb and forefinger.
- Hold your breath for as long as comfortable, nodding your head.
- Now, breathe back in through the nose, keeping the mouth closed.
- Continue to breathe gently, in and out through your nose, with mouth closed.
Immediately after doing this exercise, re-check your left and right nostril to see how clear they are. This is a good place to start for improving our breathing.
UPPER CHEST BREATHING
Upper chest breathing compared to diaphragm breathing
A normal, healthy resting breathing pattern is nasal, silent, 8-12 breaths per minute, smooth, even and regular and 80% diaphragmatic. However, it’s common today for people to breathe predominantly from their upper chest muscles, also known as the secondary respiratory muscles. This is a very tiring way to breathe because the upper chest muscles are not designed for constant use and should only engage in an emergency. They are inefficient and use up a lot of the body’s oxygen reserves and this is why they are often referred to as oxygen robbers. By contrast, the diaphragm is a powerful muscle and like the heart it never needs a rest, from your first breath to your last. Breathing mainly from the diaphragm uses just 2% oxygen while breathing mainly from the upper chest muscles uses up to 25% oxygen. Think of your upper chest muscles as your emergency back-up muscles. You do not need to use them when you are just going about your everyday life. If you think of breathing as information for the body, by breathing using mainly your emergency back-up muscles you are constantly giving your body the message that you are in danger.
Further advantages of diaphragm breathing
There are so many reasons to breathe predominantly from the diaphragm, including improved posture, reduced tension in the upper chest muscles, more efficient gas exchange, stimulation of the relaxation response and reduced blood pressure. Also, because the diaphragm plays a vital role in massaging the internal organs, breathing mainly from the diaphragm facilitates improved digestion, bowel function and movement of blood and lymphatic fluid. It is impossible overstate the importance of diaphragm breathing for health and wellbeing.
To sum up: “The diaphragm may be our muscle of respiration, but it’s more than breath. It has an impact on all major physiological systems; posture, circulation, immune function, digestion, emotional regulation – the list is long.”
Factors that contribute to people to becoming mainly chest breathers
Breathing through the mouth immediately engages the upper chest muscles and activates the sympathetic nervous system, which is the ‘fight or flight’ branch of the autonomic nervous system. Being stressed and holding tension in the belly will inhibit the diaphragm so that the upper chest muscles step in to assist the diaphragm. Having poor posture, which can include slouching or rib jutting, will also inhibit the diaphragm and contribute to upper chest breathing.
How upper chest breathing exacerbates asthma
Upper chest breathing contributes to over-breathing, which just means breathing in excess of metabolic requirements. Over-breathing (or hyperventilation) leads to a reduction of CO2 in the lungs and blood. You have over 100,000 km of tubes in the body, including the airways and all these tubes have smooth muscles wrapped around them. CO2 is a smooth muscle relaxant – it keeps airways and blood vessels open. When CO2 levels in the lungs and blood are less than ideal, it can lead to smooth muscles spasm around airways. This makes it more difficult to breathe and leads to over-engagement of the upper chest muscles which contributes to over-breathing. As you can see, there is a very vicious cycle at play. CO2 relaxes smooth muscle around airways, in the same way Ventolin does, and breathing correctly has the benefit of harnessing this natural bronchodilator. Improving your breathing pattern, including establishing nasal/diaphragm breathing, a smooth, regular even breathing pattern and normalising the amount of air you breathe can be a game changer for asthma.
How to tell if you are mainly upper chest breathing or diaphragm breathing
Put one hand on your chest and the other hand on your belly. Now tune in to your breathing for a few breaths and start to notice which hand moves most when you breathe. If it’s the upper hand then you are likely to be breathing predominantly from your upper chest muscles. Do this same exercise next time you are out walking and notice whether you tend to upper chest breathe when exercising. Also, notice what happens when you are stressed.
Another way to check is to notice whether your shoulders and upper chest rise when you breathe. If you have trouble feeling this, you could use a mirror to observe. We call this piston breathing. When you upper chest breathe, the movement of breathing is more of an up and down movement, just like a piston. When you breathe mostly using your diaphragm, the movement of breathing is more like a bellows where you get slightly bigger around your middle, just below the ribs, into the sides and the back in this area as well as out the front. When you breathe mainly from your diaphragm, there is little movement in the upper chest and the shoulders.
Another tactic is to ask someone to observe you when you are unaware and notice where most of the movement is when you breathe. One sure-fire way to tell is if you tend to have tight and sore shoulder, chest and even neck muscles. This is likely to be a sign that you are overusing these muscles and are over-breathing.
Should diaphragm breathing be big, deep and full?
No. This is the opposite of a good breathing pattern and a common misconception. People often associate diaphragm breathing with big breathing and emptying and filling the lungs, which leads to over-breathing and all the problems caused by reduced CO2 in the lungs and blood. A normal breath at rest is just 500 ml which is only ⅛ of your lung capacity. If you think of a 500 ml water bottle, that gives you an idea of just how small a normal breath is – in and out is one breath. So, diaphragm breathing done correctly is small-volume breathing.
Often when we teach diaphragm breathing there is a lot of unlearning to do where we need to dismantle the associations between diaphragm breathing and concepts such as big, deep, full, abdominal or belly breathing. These concepts lead to large-volume diaphragm breathing.
What to do if you notice you are an upper chest breather
It starts with the basics, which means having a relaxed upright posture and always breathing through the nose. The nose and the diaphragm go together and this promotes the relaxation response, whereas breathing through the mouth engages the upper chest muscles and the fight or flight response.
Next is to learn what it feels like when you diaphragm breathe. Try this:
- Sit in a firm chair in a relaxed, upright posture.
- Put one hand on your chest and the other just below your ribs.
- Now, imagine that you have a 10cm-wide band of skin all around your body just below the end of your breastbone that is gold in colour. Think of this as your soft gold band. It’s like a wide, high, soft waistband – it has give in it.
- Feel this area expand gently as you breathe in and fall back into place as you breathe out. Feel the lateral (sideways) expansion of your lower ribs as you inhale and feel the narrowing of your lower ribs as you exhale. The movement should occur at the lower end of your rib cage at the sides and back as well as in the solar plexus at the front. Remember the movement is only small.
If you are having trouble with this, try lying on your back and putting something under your knees to support them. Then do the same exercise explained above, but this time lying on your back. This takes the postural work away from the diaphragm so that you can focus on breathing. Once you have a feel for this lying down, try it sitting back on a chair.
Another useful technique that can help you to learn what it feels like when you diaphragm breathe compared to upper chest breathing is reverse practice, where you deliberately chest breathe for 2 breaths and then switch to diaphragm breathing for 2 breaths and then back to chest breathing, and so on. Deliberately engaging the bad habit helps you to get a feel for the correct habit.
These are just a few basic starting tips, and it should be pointed out that while some people will be able to establish an ideal resting 80:20 diaphragm/chest breathing pattern just with awareness, others will require help from a breathing educator.
Follow this link for additional guidelines on
diaphragmatic breathing
This article appeared in Asthma New Zealand’s June 2021 issue of O2 magazine.
Some of this information was included in interviews with Glenn White of Buteyko Breathing Clinics Auckland, and Nicky McLeod of the Breathing Clinic Nelson by Asthma New Zealand CE Katheren Leitner for World Asthma Day 4 May 2021.
Interview with Glenn on Asthma New Zealand’s YouTube Channel
Interview with Glenn on Buteyko Breathing Clinic YouTube Channel
Interview with Nicky McLeod on Asthma New Zealand’s YouTube channel
About Glenn White
Glenn runs The Buteyko Breathing Clinic in Freemans, Bay Auckland. For a large part of his life, he suffered very badly with asthma. He had been diagnosed with asthma at the age of two and since his late teens had been on daily inhaled corticosteroids and bronchodilators. Despite being very compliant with asthma medications, there were times when the asthma was life-threatening. Twenty years ago, Glenn enrolled in a Buteyko Breathing course in Newcastle in the United Kingdom. On that course he learned breathing techniques that have enabled him to control his asthma, without need for asthma medication, ever since. And it wasn’t just the asthma that resolved. For the first time in 30 years, he was able to break the cycle of bronchial infections and flare-ups of hay fever. He was astounded by the dramatic improvements in his health and decided to change careers (20 years in gold exploration) and train as a Buteyko practitioner. Glenn moved back to New Zealand and opened his clinic in 2001.
About Nicky McLeod
For 13 years Nicky was medicated for epilepsy. She had grand mal and partial complex seizures that came on after the birth of her first child. She enrolled in a Breathing Retraining Course with Glenn White in Auckland, ironically to address her husband’s snoring. She had no idea that there was anything wrong with her breathing but learnt that she was a chronic hidden hyperventilator. She breathed through her mouth all night long and half the day, breathed fast and deep, mainly using her upper chest muscles and sighed heavily throughout the day – all signs of a dysfunctional baseline breathing pattern.
The improvements in her health and wellbeing were significant as she learnt about functional breathing and started to incorporate this new knowledge. Within six months of commencing the course, she no longer needed epilepsy mediation and has been seizure free ever since. Nicky went on to train as a practitioner and establish The Breathing Clinic in Nelson. She used her knowledge to teach her husband to considerably reduce snoring and her son to breathe his way through asthma symptoms and he now no longer has asthma.
Consultations and courses
To book a consultation or course, contact our clinic and speak with a practitioner.
Tel: 09-360 6291
Posted: Thu 13 May 2021