Important considerations in management and acute care of suspected COVID-19 patients
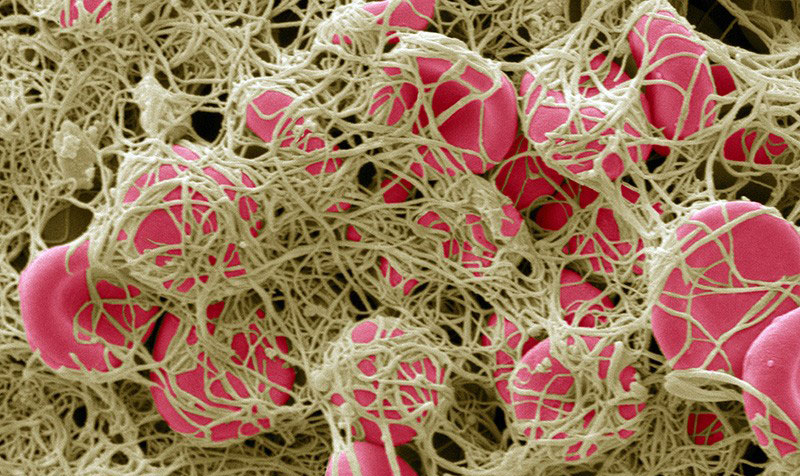
Purple rashes, pseudo frost bite, swollen legs, blood clots strokes and sudden death. Physicians working at the coal face of COVID-19 are reporting "mysterious" symptoms suggesting a phenomenon known as "silent hypoxia," where people with the virus progress from mild to severe hypoxia in the absence of air hunger.
Hypoxia is a condition or state in which the supply of oxygen is insufficient for normal life functions. In younger, healthy individuals testing positive to COVID-19 this sometimes manifests as an elevated breathing rate, faint bluish tint to fingers, lips or ears, pale complexion, chillblains, frostbite-like lesions, hives, skin rashes or thick dark-red blood, often in the absence of other symptoms. These symptoms are consistent with hypoxic states sometimes seen in high-altitude climbers and pilots. One mechanism proposed for the prolonged and progressive hypoxia seen in COVID-19 cases is the result of COVID-19 glycoproteins binding to the heme groups in haemoglobin, displacing oxygen (O2).[1]
Although the lack of air hunger accompanying hypoxia may appear mysterious, its physiology is not. While oxygen uptake and delivery may be compromised due to the virus, carbon dioxide (CO2) is still being produced. CO2 concentration and pH of arterial blood plasma and cerebrospinal fluid drive the reflex to breathe and the experience of air hunger, not the hypoxia itself. Hence, the hypoxia remains "silent", misguiding the COVID-19 victim and potentially their caregivers as to the severity of the respiratory compromise.
The chemo regulatory brainstem respiratory reflexes respond to reduced O2 concentration in arterial blood plasma (PaO2) by increasing breathing rate and/or volume. This increase in the volume of air moved leads to corresponding reductions in arterial and cerebrospinal CO2 concentrations, which continue to increase as hypoxia deepens, much as would happen when acclimatising to high altitude.
In immune-compromised individuals, hypoxia may progress to where CO2 elimination is compromised, leading to acute air hunger, feelings of suffocation, extreme struggle in breathing (trauma), and an emergency trip to the hospital. Up until this point, breathing many have appeared "normal", but now it quickly deteriorates.
Severe hypocapnia for long periods of time can increase the likelihood of stroke and blood clotting, both of which are identified as COVID and very high-elevation illness outcomes.
What can we do?
Effective treatment requires early detection. Symptoms like "frostbite toes", chillblains, increased breathing rate, mouth breathing, uncharacteristic breathlessness at rest or during exertion and an elevated temperature warrant a visit to the GP. If these or other signs are present, pulse oximetry in the low 90s or less may confirm diagnosis.
In severe cases, supplemental oxygen is an essential treatment as it helps to bypass compromised haemoglobin. Some physicians in China and the US are using protocols that include hydroxychloroquine which is believed to prevent the COVID-19 glycoproteins binding to the heme groups in the red blood cells. [2],[3] This and supplemental O2 with low-flow CPAP have been successful in avoiding the need for mechanical ventilation. [4]
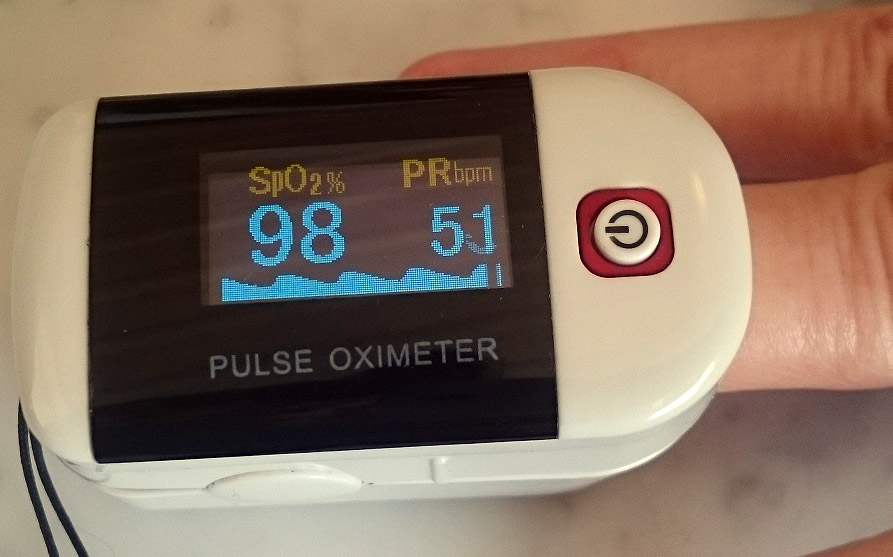
Fingertip pulse oximetry showing oxygen saturation of haemoglobin on left (normal range is 96-98% saturation).
In addition to these treatments, patients should be advised on functional breathing including instruction to nasal breathe, use of the diaphragm and to breathe at the lowest comfortable volume. Advice should not include instruction on deep breathing which can further exacerbate hypocapnia.
Breathing exercises that focus on gentle low-volume nasal breathing and diaphragm breathing can help restore functional breathing and reduce hypocapnia. In addition to this, humming has been shown to raise nitric oxide (NO) levels in the nasal sinuses. NO has potent immune boosting and germicidal properties. It also has an essential role in cardiovascular health and importantly for COVID-19, inhibits thrombosis and promotes blood flow.[5] Follow this link for more information on NO, and a humming exercise to boost NO levels.
Post COVID-19 considerations
Breathing regulates fundamental body chemistry, including extracellular pH, electrolyte balance, vascular activity (blood flow), kidney function, haemoglobin chemistry, nitric oxide production, muscle function, and neurochemical regulation. It does so by regulating the concentration of CO2 in arterial blood plasma and cerebrospinal fluid along with the pH of these fluids and the oxygen concentration in arterial plasma from moment to moment, from breath to breath. Disturbing the brainstem reflexes that regulate this basic chemistry means immediate and long-term consequences.
Unconsciously triggered breathing habits during COVID-19 may seriously compromise patients long term. CO2 deficiency, known as hypocapnia, has severe effects on physiology and associated physical and mental performance. For this reason, assessment for breathing dysfunction, including capnography and, where appropriate, breathing retraining are an important consideration in rehabilitation of patients recovering from COVID-19. Capnography and pulse oximetry are useful tools in the diagnosis of hypocapnia and assessment and retraining of dysfunctional breathing.
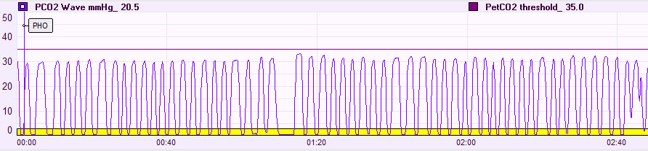
Figure shows a capnograph trace for a client with dysfunctional breathing and hypocapnia (CO2 deficit). Normocapnic = Et CO2 35-45 mm Hg
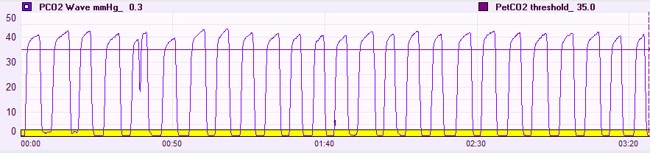
Figure shows the capnograph trace for a client with a functional breathing pattern and normal CO2 levels. Normocapnic = Et CO2 35-45 mm Hg
Read more about capnography »
Booking consultations
To book a consultation, contact our clinic and speak with a practitioner.
Tel: 09-360 6291
About this Post
The New Zealand Government, front-line workers in our hospitals and our fellow New Zealanders are doing an exemplary job in containing the spread of this virus.
Please note neither this post/blog nor any linked articles replace or negate official advice to limit the spread of COVID-19. However, now more than ever it makes sense both for physical and psychological reasons to take any steps that may improve our health. Like the advice to wash our hands frequently, there are ways to boost natural immunity which give us a sense of control, helping reduce the stress, and this is good for our immune system.
Written by Glenn White, BSC, MBIBH, BBEA, Breathing Educator
Adapted from an article and conversations with Peter Litchfield PhD, 14 May 2020
Sources and References
- Liu W, Li, H., COVID-19 Attacks the 1-Beta Chain of Hemoglobin and Captures the Porphyrin to Inhibit Human Heme Metabolism. ChemRxiv 25.04.2020.
https://chemrxiv.org/articles/COVID-19_Disease_ORF8_and_Surface_Glycoprotein_Inhibit_Heme_Metabolism_by_Binding_to_Porphyrin/11938173 - Frontline COVID-19 Critical Care Working Group [https://covid19criticalcare.com]
- Gao J, Tian ZS, Yang X Breakthrough: Chloroquine phosphate efficacy in treatment of COVID-19 associated pneumonia. Biosci Trends. 2020 Mar 16
https://www.ncbi.nlm.nih.gov/pubmed/32074550 - UCL-Ventura breathing aids for Covid-19 patients
https://www.ucl.ac.uk/healthcare-engineering/covid-19/ucl-ventura-breathing-aids-covid-19-patients - Ghimire K et al. Nitric oxide: what's new to NO? Am J Physiol Cell Physiol. 2017 https://www.ncbi.nlm.nih.gov/pubmed/27974299
Posted: Mon 18 May 2020