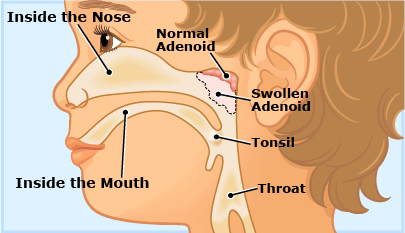
The adenoids are a mass of soft tissue behind the nasal cavity. Like lymph nodes, adenoids are part of the immune system and are made of the same type of tissue. Adenoids start growing from birth and reach their peak size when the child is between about 3 and 5 years of age. After the age of 7 they shrink, and are barely detectable during adolescence. They have disappeared completely by adulthood.
Babies and very young children have undeveloped immune systems. At that age the adenoids are an important back up for fighting off infections. From adolescence, the immune system is better developed and they are not needed.
Your tonsils are two round, fleshy masses in the back of your throat (pharynx). Part of your immune system, your tonsils are like lymph nodes. Because of their location at the throat and palate, they can stop germs entering the body through the mouth or the nose. The tonsils also contain a lot of white blood cells, which are responsible for killing germs.

It has even been suggested that the tonsils are the site of a “natural” vaccination processes. This is why children instinctively put everything they can into their mouths and reinforces that early childhood exposure to particular microorganisms protects against allergies by properly tuning the immune system.
Read more: Why do we have tonsils? »
Enlarged Adenoids / Tonsils
Swollen or infected adenoids and tonsils can make it difficult for your child to breathe. Possible symptoms include:
- difficulty breathing through the nose (nasal obstruction)
- snoring and trouble getting a good night's sleep
- episodes of not breathing during sleep (sleep apnoea)
- sore throat and trouble swallowing
- swollen glands in the neck
- ear problems, glue ear, chronic ear infections
Enlarged adenoids can be confirmed by inspection and or x-ray. Enlarged tonsils, due to their position on the back of the throat, can usually be confirmed by visual inspection.
If your child has been diagnosed with enlarged adenoids or tonsils, it is likely that surgical removal may have been advised by your paediatrician. Enlargement can be sufficient to cause a blockage of the nose making nasal breathing difficult or impossible. Chronic infection may also lead to ear problems including glue ear. These problems are seen by doctors as being indicative of dysfunctional adenoids with surgical removal being the best option for recovery.
There are potential side-effects associated with removal. Aside from the obvious stress of having your child undergo surgery, it is common for children to be left even more susceptible to respiratory infections following removal. This has been confirmed by a 2013 study that concluded: In children selected for adenoidectomy for recurrent URTIs, immediate adenoidectomy results in an increase in costs, whereas it confers no clinical benefit over an initial watchful waiting strategy.1
A 2018 study of almost 1.2 million children, of whom 17 460 had adenoidectomy, 11 830 tonsillectomy, and 31 377 adenotonsillectomy surgeries found associated increases in long-term risks of respiratory, infectious, and allergic diseases. The authors advised the importance of considering long-term risks when making decisions to perform tonsillectomy or adenoidectomy.2
Adenoidectomy / Tonsillectomy – is there a better option?
The Buteyko Breathing Clinic programme is a safe and effective alternative to adenoid/tonsillectomy.
 It is widely accepted that children with enlarged adenoids or tonsils tend to be habitual ‘mouth-breathers’. However, contrary to popular thinking, habitual open-mouth breathing may in fact be the reason the adenoids and tonsils become enlarged in the first place. Once enlarged, nose breathing becomes even more difficult. Affected children develop a habitual mouth-breathing habit and this can result in craniofacial changes, including narrowing of the airway, leading to chronic nasal congestion and other upper airway disorders. The key to resolving this problem is in recognising that the mouth-breathing habit comes first. So, correcting the underlying dysfunctional breathing pattern is the first step to consider in reducing adenoids and making breathing easier.
It is widely accepted that children with enlarged adenoids or tonsils tend to be habitual ‘mouth-breathers’. However, contrary to popular thinking, habitual open-mouth breathing may in fact be the reason the adenoids and tonsils become enlarged in the first place. Once enlarged, nose breathing becomes even more difficult. Affected children develop a habitual mouth-breathing habit and this can result in craniofacial changes, including narrowing of the airway, leading to chronic nasal congestion and other upper airway disorders. The key to resolving this problem is in recognising that the mouth-breathing habit comes first. So, correcting the underlying dysfunctional breathing pattern is the first step to consider in reducing adenoids and making breathing easier.
We will teach your child easy-to-learn breathing exercises which include games. This helps to normalise their breathing making nasal breathing easier. In some cases, dietary changes may be recommended to help with the process.
Adenoid reduction, and with it the ability to nose breathe, is often seen in the first week of the programme. In many cases, adenoids return to normal size, within weeks, eliminating the need for surgery. We encourage all parents of children with swollen adenoids and chronic nasal congestion to consider the Buteyko breathing programme before embarking on invasive and potentially unnecessary surgery.

Within days our daughter was able to breathe through her nose. This is something she hadn’t done for years. It is two months now since she did the course. Her adenoids have returned to their normal size and she now breathes through her nose most of the time, not all.
Mareea – Read more »

Josie attended the Buteyko breathing course and within one month, her tonsils were down to their normal size. Her continual stuffy nose has cleared and her sporting abilities have improved respectively.
Susan Clow BDS Otago (Retired) – Read more »


